Dyskinesia in Parkinson’s Disease refers to involuntary, uncontrolled movements that often develop after long-term use of Parkinson’s medications—especially levodopa. While these movements can look concerning, they’re actually a common and manageable part of the disease for many patients.
If you’re trying to understand dyskinesia, there are three key questions to answer: what causes it, how to recognize it, and how to manage it effectively. Most cases are linked to medication response over time rather than the disease itself. Still, symptoms can vary widely—from mild restlessness to more noticeable, full-body movements.
You may also be wondering how dyskinesia differs from other Parkinson’s symptoms like tremor or stiffness. This distinction matters because treatment decisions depend on it. Managing dyskinesia is often about balance—reducing unwanted movement without worsening other symptoms.
So how do you actually manage it in real life? Below, we break it down step by step—from definition to treatment strategies—so you can better understand what’s happening and what to do next.
What Is Dyskinesia in Parkinson’s Disease?
Dyskinesia is a movement complication of Parkinson’s treatment characterized by involuntary, irregular movements that occur most often during peak medication effect.
In simple terms, it’s when your body moves in ways you didn’t intend—such as swaying, twisting, fidgeting, or jerking. These movements can affect different parts of the body, including the arms, legs, trunk, face, or neck.
This happens because Parkinson’s medications—especially levodopa—restore dopamine levels in the brain. Over time, however, the brain becomes more sensitive to fluctuations in dopamine. That’s when dyskinesia can appear.
Is Dyskinesia a Symptom or a Side Effect of Parkinson’s Disease?
Dyskinesia is primarily a side effect of treatment, not a core symptom of Parkinson’s disease.
However, it’s not just about the medication. Parkinson’s itself changes how the brain processes dopamine. As the disease progresses, the brain becomes less able to regulate dopamine smoothly. When medication is added to that mix, it can lead to overstimulation—resulting in involuntary movements.
So in reality, dyskinesia is caused by both the disease and the treatment working together over time.
What Types of Dyskinesia Occur in Parkinson’s Patients?
There are three clinically important dyskinesia patterns: peak-dose dyskinesia, diphasic dyskinesia, and off-period dystonia, classified by their timing relative to medication effect.
- Peak-dose dyskinesia tends to happen when levodopa effect is strongest.
- Diphasic dyskinesia appears as medication starts working or wears off.
- Off-period dystonia more often occurs when medication effect is low, especially in the early morning.
These distinctions are not academic; they shape whether clinicians reduce a dose, split dosing, change formulation, or consider advanced therapy.
What Causes Dyskinesia in Parkinson’s Disease?
Dyskinesia is mainly caused by long-term use of levodopa combined with changes in the brain’s dopamine system as Parkinson’s progresses.
Over time, dopamine-producing neurons continue to decline. Without those neurons to buffer dopamine levels, the brain experiences sharper “peaks and dips” when medication is taken. These fluctuations can trigger abnormal signaling in motor pathways.
Other factors can increase the risk of dyskinesia:
- Longer duration of treatment
- Younger age at Parkinson’s onset
- Higher or more frequent levodopa doses
Long-term observational and review data show dyskinesia becomes more common with time on levodopa. A JAMA Neurology study estimated dyskinesia rates at about 30% by 5 treatment years and 59% by 10 years, while other reviews commonly cite roughly 40% to 50% after 5 years and a majority by 10 years. The exact number varies by study design and patient mix, but the directional pattern is consistent.
Does Levodopa Cause Dyskinesia in Parkinson’s Disease?
Yes, levodopa is the treatment most strongly associated with dyskinesia, especially after prolonged use, higher cumulative exposure, or in patients with younger-onset disease.
That said, levodopa is still the most effective treatment for improving Parkinson’s symptoms like stiffness and slow movement. Dyskinesia doesn’t mean the medication is wrong—it simply means the treatment may need adjustment.
Parkinson’s Foundation and APDA both explain that levodopa is standard therapy and that dyskinesia is a known complication of treatment.
Why Does the Brain Develop Dyskinesia Over Time?
The brain develops dyskinesia because dopamine signaling becomes unstable as Parkinson’s progresses.
In a healthy brain, dopamine is released steadily. In Parkinson’s, dopamine levels depend heavily on medication timing. This creates a “pulsing” effect instead of a smooth flow.
Over time, this pulsatile stimulation changes how brain cells respond—making them more sensitive and more likely to trigger involuntary movements.
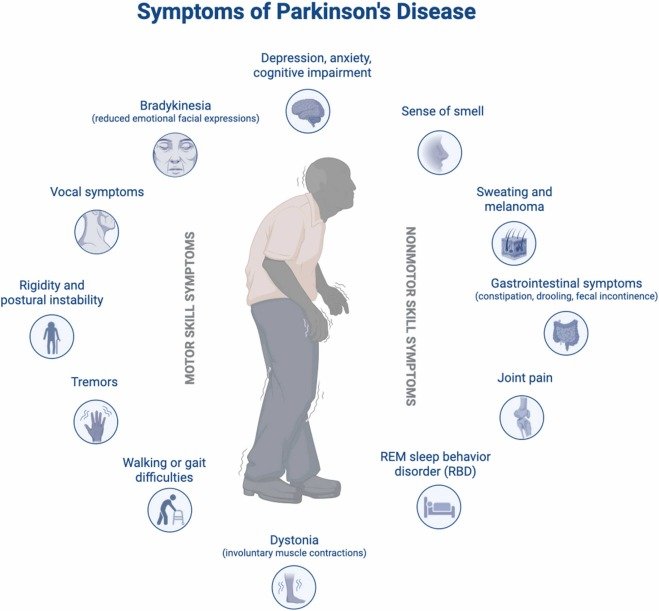
What Are the Symptoms of Dyskinesia in Parkinson’s Patients?
Dyskinesia symptoms include involuntary, flowing movements such as twisting, swaying, writhing, or jerking that can affect different parts of the body.
These movements can range from subtle to severe. Some patients barely notice them, while others find they interfere with daily activities like walking, eating, or writing.
Common symptoms include:
- Jerking motions in arms or legs
- Fidgeting or restlessness
- Head bobbing or swaying
- Twisting movements of the torso
How Can You Recognize Dyskinesia vs Tremor in Parkinson’s?
Dyskinesia is irregular and flowing, while tremor is rhythmic and repetitive.
Tremors usually happen when muscles are at rest and follow a steady pattern. Dyskinesia, on the other hand, looks more unpredictable and often occurs when medication is working (during “on” time).
This difference is important because treating tremor and dyskinesia requires different strategies.
When Do Dyskinesia Symptoms Typically Appear?
Dyskinesia typically appears after several years of treatment and often during peak medication effect.
In many patients, symptoms follow a predictable pattern:
- During peak-dose → more movement
- During wearing-off → less movement but more stiffness
Tracking when symptoms occur can help doctors adjust treatment more effectively.
How Can Dyskinesia in Parkinson’s Disease Be Managed or Treated?
Dyskinesia can be managed using three main approaches: medication adjustments, targeted therapies, and advanced treatments like surgery.
The goal isn’t just to eliminate movement—it’s to find the right balance between mobility and control.
What Medications Help Reduce Dyskinesia in Parkinson’s?
The main medication option is amantadine, while levodopa regimen adjustments and formulation changes may also reduce dyskinesia burden.
To make that actionable, clinicians may reduce individual levodopa doses, divide doses more evenly, or shift to formulations designed to smooth dopamine exposure. Parkinson’s Foundation and Michael J. Fox Foundation both note these timing and formulation strategies. NINDS and Cleveland Clinic also identify amantadine as a drug that can reduce levodopa-induced dyskinesia.
A useful evidence point is that a controlled study reported amantadine was effective against dyskinesia in roughly 60% to 70% of patients. That does not mean every patient will benefit or tolerate it well, but it explains why amantadine remains central in dyskinesia management discussions.
Can Lifestyle Changes Help Manage Dyskinesia Symptoms?
Yes, lifestyle changes can help improve overall function and reduce the impact of dyskinesia.
Helpful strategies include:
- Regular exercise (improves motor control)
- Structured daily routines
- Stress management
- Physical or occupational therapy
While these won’t eliminate dyskinesia, they can make symptoms more manageable.
Alongside lifestyle adjustments and rehabilitation therapies, some individuals explore assistive tools that enhance stability during everyday tasks. Wearable mechanical solutions like GyroGlove use gyroscopic resistance to help steady hand movement in real time, supporting activities such as eating or writing. While not a treatment for dyskinesia itself, these technologies can play a meaningful role in improving functional independence and quality of life.
How Effective Is Surgical Treatment Like Deep Brain Stimulation?
Deep brain stimulation (DBS) is highly effective for selected patients with severe dyskinesia or motor fluctuations.
DBS works by sending electrical signals to specific brain areas that control movement. It can reduce both dyskinesia and “off” time. However, it’s typically considered only when:
- Symptoms significantly affect quality of life
- Medications no longer provide stable control
Mayo Clinic explains that DBS uses implanted electrodes to modulate brain activity, and NHS-linked specialty guidance notes DBS may be used in later-stage Parkinson’s to treat tremor and dyskinesia. Comparative literature also suggests target choice matters, with some evidence that GPi DBS may reduce dyskinesia more than STN DBS at 12 months in advanced Parkinson’s disease.
How Does Dyskinesia Differ Across Parkinson’s Stages and Treatment Strategies?
Dyskinesia changes over time because Parkinson’s progression and treatment adjustments affect how symptoms appear and respond.
In early stages, dyskinesia may be mild and occasional. In later stages, it can become more frequent and harder to balance with medication needs.
What Is the Difference Between Peak-Dose and Diphasic Dyskinesia?
Peak-dose dyskinesia happens when medication is strongest, while diphasic dyskinesia occurs as medication levels rise or fall.
This difference matters because treatment strategies vary:
- Diphasic → adjust timing or frequency
- Peak-dose → reduce dose or smooth delivery
How Does Deep Brain Stimulation Compare to Medication Adjustment?
Medication adjustment is first-line treatment, while DBS is used when medication no longer works well enough.
In general:
- DBS → more stable control but requires surgery
- Medication → flexible, non-invasive
Can Adjusting Medication Timing Reduce Dyskinesia Without Surgery?
Yes, adjusting medication timing can reduce dyskinesia because it helps stabilize dopamine levels throughout the day.
Many patients improve by:
- Aligning medication with meals and activity
- Taking smaller, more frequent doses
Are There Emerging Treatments or Research Trends for Dyskinesia?
Yes, research is exploring new drug therapies, gene-based treatments, and improved dopamine delivery systems.
Scientists are also studying why some patients develop dyskinesia earlier than others, which may lead to more personalized treatment in the future.
Final Takeaway
Dyskinesia in Parkinson’s disease is a common but manageable complication of long-term treatment. Understanding its causes, recognizing its symptoms, and applying the right treatment strategies can significantly improve quality of life.
The most important step is working closely with a neurologist to find the right balance between medication effectiveness and side effects.
Important medical note: this article is informational and should not replace diagnosis or treatment planning with a neurologist or movement-disorder specialist, especially when medication changes, falls, hallucinations, or sudden worsening are involved.
Sources:
- https://www.parkinson.org/understanding-parkinsons/movement-symptoms/dyskinesia
- https://pmc.ncbi.nlm.nih.gov/articles/PMC2600052/
- https://www.parkinsons.org.uk/information/drugs/side-effects/dyskinesia-wearing-off
- https://www.nhs.uk/conditions/parkinsons-disease/treatment/
- https://www.michaeljfox.org/news/dyskinesia
- https://pubmed.ncbi.nlm.nih.gov/21217832/
- https://www.mayoclinic.org/tests-procedures/deep-brain-stimulation/about/pac-20384562
- https://www.parkinson.org/library/podcast/97
- https://pubmed.ncbi.nlm.nih.gov/23931952/
- https://www.frontiersin.org/journals/aging-neuroscience/articles/10.3389/fnagi.2025.1684885/full